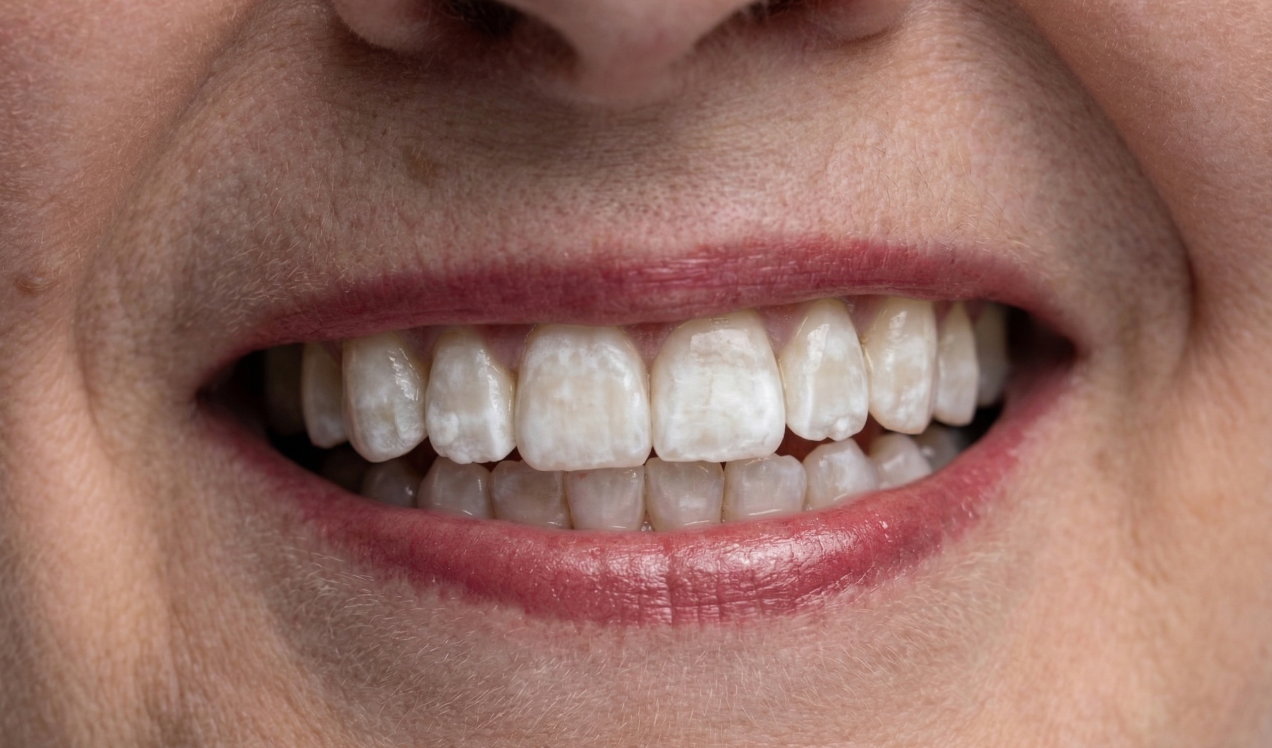
Noticed chalky patches, white blotches, or small white dots on your teeth? You’re not alone. White marks on teeth are one of the most common cosmetic concerns we see, and they affect both children and adults.
The good news is they’re usually not an emergency. The less straightforward news is that appearance alone can’t tell you the cause. Some white spots are purely cosmetic and have been there since childhood. Others are early signs of mineral loss that, left unchecked, can progress to cavities and bigger problems down the track.
The cause matters because it changes what you should do about it. A white spot from fluorosis needs a completely different approach to one caused by early decay. And some white marks that look concerning are actually stable and don’t need treatment at all.
This guide breaks down why white discolouration appears on teeth, how to tell whether yours needs attention, and what your treatment options look like, from the most conservative through to cosmetic solutions.
What causes white marks on teeth?
White spots, patches, and blotches can show up for several different reasons. Understanding which one applies to you is the first step toward knowing whether treatment is needed or whether monitoring is enough.
Early demineralisation
This is the most important cause to recognise because it’s the one that can get worse. Demineralisation is the first visible stage of enamel breakdown, where acids produced by bacteria dissolve minerals out of the tooth surface. The affected area looks matte, chalky, or opaque compared to the surrounding enamel. At this stage the surface is still intact, which means the process can sometimes be slowed or reversed with the right care. Left alone, it can progress into a full cavity.
Fluorosis
Fluoride is essential for strong teeth, but too much during childhood development can leave permanent white flecks or streaks in the enamel. This is called dental fluorosis. In Australia, most tap water is fluoridated at a controlled level, so fluorosis here tends to be mild. It’s more commonly seen when young children swallow toothpaste regularly or use adult-strength fluoride products too early. The marks are usually symmetrical across matching teeth and don’t change over time.
Enamel hypoplasia
Sometimes the enamel simply doesn’t form properly during childhood. High fevers, nutritional deficiencies, premature birth, or illness during key developmental stages can all disrupt enamel formation. The result is patches of thinner or softer enamel that appear whiter or more opaque than the surrounding tooth. This isn’t caused by anything the patient did wrong. These marks are stable but can make the affected areas more vulnerable to wear and decay over time.
White spots after braces
One of the most common times people notice white marks is after orthodontic brackets come off. When cleaning around braces is difficult, plaque builds up against the enamel and causes localised demineralisation. The white patches typically sit in a pattern matching where the brackets were bonded. For teens and parents, this is worth knowing about before and during orthodontic treatment, not just after.
Acid erosion from diet
Frequent exposure to acidic foods and drinks, think soft drinks, energy drinks, citrus, sports drinks, and even kombucha, can soften and erode enamel over time. As the enamel thins or loses minerals, it changes how light reflects off the surface, creating a chalky or uneven appearance. This is different from a single cavity forming in one spot. Acid erosion tends to affect broader areas, particularly the front surfaces of teeth.
Dry mouth and mouth breathing
This one often gets overlooked. When saliva flow drops, whether from mouth breathing during sleep, certain medications, or chronic nasal congestion, the teeth lose their natural protective coating. Enamel can appear temporarily chalky or develop white patches from dehydration. In children who habitually breathe through their mouth, this can become an ongoing issue that affects enamel development. If your child snores or sleeps with their mouth open, it’s worth mentioning at their next dental visit.
Are white spots a sign of something serious?
Not always, but sometimes. The key is knowing what to look for so you can tell the difference between a cosmetic issue and an early warning sign.
Likely cosmetic and stable: White marks that have been present since childhood, appear symmetrical across matching teeth, and haven’t changed in size or colour over time are usually fluorosis or enamel hypoplasia. These don’t typically need treatment unless the appearance bothers you.
Worth monitoring: A single white spot on an otherwise healthy tooth, particularly near the gumline, may be early demineralisation. If the surface still feels smooth and there’s no sensitivity, this is the stage where remineralisation strategies can make a real difference. Your dentist can track these with clinical photos at regular check-ups to make sure they’re not progressing.
Book an assessment: If you notice a white spot that feels rough to your tongue, catches food, comes with sensitivity to hot or cold, or has started shifting to brown or grey, the enamel surface has likely broken down. At that point it’s no longer an early warning. It’s a cavity that needs a restoration. The sooner it’s assessed, the more conservative the treatment can be.
The honest answer is that you can’t reliably diagnose the cause of white marks yourself. Photos online make everything look the same. A clinical examination with X-rays tells you what’s actually going on beneath the surface and whether anything needs to happen. Once you know the cause, treatment can be matched to your specific situation.
Why DIY whitening isn't always the right first step?
It’s a reasonable instinct. You see white patches, so you reach for a whitening product to even things out. But bleaching works by lightening the surrounding enamel, which can actually make white spots more obvious in the short term, not less.
More importantly, if the white marks are caused by weakened or demineralised enamel, applying peroxide-based products to an already compromised surface isn’t ideal. You want that enamel assessed and strengthened first, not stripped further.
This doesn’t mean professional teeth whitening is off the table. It can work well as part of a broader plan once the underlying cause is understood and any active enamel issues have been addressed. The order just matters. Diagnose first, then decide on cosmetic steps with your dentist rather than the other way around.
How white spots are treated?
Treatment depends on what’s causing the white marks and how deep the changes go. Your dentist will always start with the most conservative option and only move to more involved treatments if needed.
Remineralisation
For early demineralisation where the enamel surface is still intact, the goal is to put minerals back in and stop the process from progressing. This might include high-concentration fluoride treatments applied in the chair, take-home products containing CPP-ACP (calcium and phosphate compounds, like Tooth Mousse), and adjustments to your oral hygiene and diet. Remineralisation takes time and consistency, but it’s the least invasive path and can make a genuine difference when white spots are caught early.
Resin infiltration
This is a relatively newer option that works well for post-braces white spots and superficial demineralisation. A tooth-coloured resin is applied to the porous enamel, filling in the affected area and blending the colour with the surrounding tooth. There’s no drilling involved, no anaesthetic needed, and it can often be done in a single visit. It won’t help with every type of white spot, but for the right cases it gives a noticeably better cosmetic result with minimal intervention.
Microabrasion
For surface-level discolouration, particularly mild fluorosis, microabrasion gently polishes away a thin outer layer of enamel using a mild abrasive compound. This can reduce or remove shallow white patches without affecting the deeper tooth structure. It’s quick and straightforward, but it only works where the discolouration is confined to the outermost enamel layer.
Composite bonding and tooth-coloured restorations
Where the enamel has broken down into a cavity, or where white marks are too deep for conservative approaches, a tooth-coloured composite restoration can repair the area and restore a natural appearance. This is the same material used in white fillings, shaped and polished to match your surrounding teeth.
Veneers
For significant cosmetic concerns affecting multiple front teeth, porcelain veneers offer a more comprehensive solution. A thin shell is bonded over the front surface of each tooth, covering white patches, uneven colour, and other imperfections in one step. Veneers are a bigger commitment than the options above, so they’re typically considered when conservative approaches haven’t achieved the result you’re after.
Preventing white spots
Better still, some white spots can be avoided altogether. Generic “brush and floss” advice isn’t particularly helpful here, so let’s be more specific.
If your child is in braces or clear aligners or about to start orthodontic treatment, cleaning thoroughly around brackets and wires is the single biggest thing that prevents post-braces white marks. An electric toothbrush and interdental brushes make a real difference. For younger children, supervise brushing and use only a pea-sized amount of age-appropriate fluoride toothpaste. Swallowing excess toothpaste over time is one of the most common causes of mild fluorosis.
Cut back on frequent sipping and snacking on acidic drinks and foods. It’s not about eliminating them entirely, it’s about reducing how often your teeth are exposed throughout the day. Water between meals helps neutralise acid.
If your child breathes through their mouth during sleep or snores regularly, mention it at their next dental or GP visit. Chronic mouth breathing dries out enamel and can contribute to white spot development over time.
When to book an assessment
If you’ve noticed white marks and you’re unsure whether they’re cosmetic or something that needs attention, an examination with X-rays gives you a clear answer. We’ll explain what’s causing them, whether they need treatment or just monitoring, and what your options are if you’d like to improve the appearance.
There’s no judgement in the question and no pressure to commit to treatment on the spot. Book a consultation with our Gisborne team and we’ll take it from there.
Frequently asked questions
It depends on the cause. White marks from temporary enamel dehydration, like sleeping with your mouth open, will typically disappear once saliva rehydrates the tooth surface. Early demineralisation spots can improve with remineralisation strategies such as fluoride treatments and CPP-ACP products, though they may not vanish completely. White marks caused by fluorosis or enamel hypoplasia are permanent structural changes and won’t fade on their own, but cosmetic treatments can reduce their appearance.
They can be. A chalky white spot, particularly near the gumline, is often the earliest visible sign of enamel breakdown. At this stage the surface is still intact and the process may be reversible with the right care. Once the spot feels rough, catches food, or starts changing to brown or grey, the enamel has broken through into a cavity that needs a restoration. That’s why getting white marks assessed early matters.
Not always, and it can sometimes make them more noticeable. Whitening works by lightening the surrounding enamel, which can increase the contrast with the white patches rather than blending them. Professional whitening can still be part of the solution, but it works best when combined with other treatments and after the underlying cause has been assessed. Your dentist can advise on the right sequence for your situation.
Plaque that builds up around orthodontic brackets produces acid against the enamel surface. If cleaning is difficult during treatment, this causes localised demineralisation, leaving white marks in a pattern matching where the brackets sat. It’s one of the most common causes of white spots in teens. Using an electric toothbrush, interdental brushes, and a fluoride rinse during orthodontic treatment significantly reduces the risk.
Many white spots are preventable. Supervise brushing in younger children and use only a pea-sized amount of age-appropriate fluoride toothpaste to reduce the risk of fluorosis. During orthodontic treatment, prioritise thorough cleaning around brackets and wires. Limit frequent snacking on acidic or sugary foods and drinks. And if your child breathes through their mouth during sleep, raise it with your dentist or GP, as chronic mouth breathing can affect enamel development.
If you’ve noticed white marks that are new, changing, rough in texture, or accompanied by sensitivity, book an assessment sooner rather than later. Even if the spots turn out to be cosmetic, a clinical examination with X-rays is the only reliable way to confirm the cause and rule out early decay. The earlier a problem is identified, the more conservative the treatment.